
Blood sugar crash symptoms can feel sudden, intense, and confusing. One minute you feel completely fine — the next you’re shaky, tired, irritable, and desperately hungry. Many people assume they just need more caffeine or that they didn’t sleep enough. But in reality, blood sugar crash symptoms are often caused by a rapid drop in glucose levels after a spike, triggering a stress response inside your body.
When blood sugar rises quickly — especially after refined carbohydrates or sugary foods — insulin is released to move glucose out of the bloodstream and into cells. If insulin lowers glucose too aggressively, levels can fall sharply. That sudden decline activates stress hormones like adrenaline and cortisol, creating the uncomfortable cluster of blood sugar crash symptoms people describe as shakiness, brain fog, sweating, anxiety, and sudden exhaustion.
According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), glucose is the body’s primary energy source and must remain within a stable range for optimal function. Understanding what disrupts that stability is the key to preventing crashes.
What Happens When Your Blood Sugar Drops Too Fast
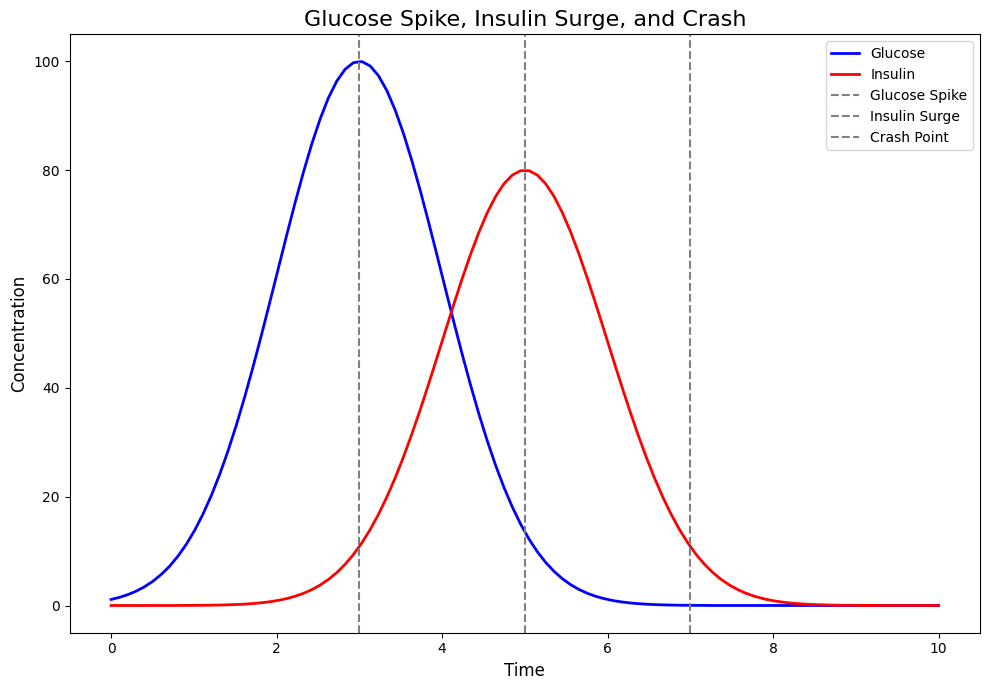
Glucose enters the bloodstream after you eat carbohydrates. The pancreas releases insulin, allowing glucose to enter cells for energy or storage.
The issue begins when blood sugar rises too quickly.
Highly refined carbohydrates — white bread, pastries, soda, sugary cereal — digest rapidly. This creates a sharp glucose spike. In response, insulin rises sharply as well.
If insulin response overshoots, glucose drops rapidly. This triggers blood sugar crash symptoms.
The body activates a counterregulatory response:
- Adrenaline increases
- Cortisol rises
- Glucagon signals the liver to release stored glucose
The Mayo Clinic explains hypoglycemia as a condition where blood sugar falls too low, activating stress hormones that cause shakiness, sweating, and weakness. Even milder, non-clinical drops can trigger similar sensations.
This explains why blood sugar crash symptoms often include:
- Shakiness
- Sweating
- Rapid heartbeat
- Sudden fatigue
- Brain fog
- Intense hunger
It’s a stress response to unstable fuel supply.
The Real Cause of Blood Sugar Crash Symptoms After Eating
Many people experience blood sugar crash symptoms 1–3 hours after eating.
Common triggers include:
- High-glycemic meals
- Low protein intake
- Low fiber meals
- Sugary beverages
- Large carb-only snacks
If you’ve ever wondered why you feel tired after eating, glucose variability is often part of the answer.
For example:
Breakfast: Sweet cereal + juice → spike → insulin surge → mid-morning crash
Lunch: White pasta + soda → spike → drop → afternoon fatigue
This pattern is sometimes referred to as reactive hypoglycemia. According to Mayo Clinic, reactive hypoglycemia (also called postprandial hypoglycemia) is a drop in blood sugar that occurs within a few hours after eating, often causing shakiness, light-headedness, sweating, hunger, or fatigue.
The cycle becomes:
Spike → crash → crave → spike again.
Without structural changes, blood sugar crash symptoms repeat daily.
Why Shakiness, Brain Fog, and Sudden Fatigue Occur Together

The brain consumes approximately 20% of your body’s glucose supply. When glucose availability drops, cognitive performance declines quickly.
Brain fog develops because neurons require steady glucose. Without it, thinking slows.
At the same time, adrenaline increases. Adrenaline causes trembling, sweating, and internal restlessness. This is why blood sugar crash symptoms can resemble anxiety.
If you’ve experienced feeling shaky and tired suddenly, glucose instability may be contributing.
Fatigue occurs because cells temporarily lack accessible fuel. The combination of stress hormone activation and low cellular energy creates the “wired but exhausted” sensation.
The Hidden Link Between Insulin Spikes and Energy Crashes
Insulin sensitivity strongly influences blood sugar crash symptoms.
Sleep deprivation reduces insulin sensitivity. According to Sleep Foundation, insufficient or poor quality sleep can impair how the body uses insulin and negatively affect blood sugar regulation, increasing the risk of glucose instability and metabolic issues.
Chronic stress elevates cortisol, altering glucose metabolism. This may explain why people who feel wired but tired at night often experience unstable energy during the day.
Blood sugar crash symptoms reflect the interaction of:
- Meal composition
- Hormonal balance
- Sleep quality
- Stress load
- Physical activity
Energy stability requires balance across all these systems.
What Most People Miss About Blood Sugar Crash Timing
Crashes don’t always happen immediately after meals.
Common timing patterns include:
Immediate crash (within 60 minutes) — often linked to liquid sugar.
Delayed crash (2–4 hours later) — classic reactive drop.
Fasting crash (after long gaps without food) — occurs when glycogen stores decline.
Many people experience a crash around mid-afternoon. If you’ve ever felt exhausted at 3PM even after 8 hours of sleep, blood sugar variability may be a contributing factor.

Tracking when blood sugar crash symptoms occur can reveal important patterns.
The Difference Between a Normal Energy Dip and a True Glucose Crash
Not every afternoon slump is a blood sugar crash. Circadian rhythm naturally creates mild dips.
A true glucose crash involves rapid physiological changes.
Blood Sugar Crash Severity Scale
| Level | Biological Pattern | Symptoms | Recovery |
|---|---|---|---|
| Mild Dip | Gradual decline | Mild hunger, slight fatigue | Balanced meal |
| Moderate Crash | Rapid insulin-driven drop | Shaky, irritable, brain fog | Protein + fiber + complex carbs |
| Severe Crash | Near hypoglycemia | Sweating, confusion, weakness | Fast carbs + evaluation |
If you regularly experience crashes, reviewing your afternoon energy crash prevention plan can help.
The Impact of Repeated Blood Sugar Crashes on Long-Term Energy Stability
Repeated blood sugar crash symptoms increase stress hormone activation.
Over time, this may:
- Increase cravings
- Elevate cortisol levels
- Promote overeating
- Reduce metabolic flexibility
- Disrupt mood stability
Choosing balanced, protein-rich snacks between meals can help prevent repeated glucose swings and reduce the intensity of blood sugar crash symptoms.

Unstable glucose curves make consistent energy difficult.
Incorporating balanced snacks like those listed in high-protein snacks under 200 calories can help stabilize blood sugar between meals.
The Science Behind Why Blood Sugar Crash Symptoms Feel So Intense
The brain constantly monitors glucose levels. When levels fall quickly, glucose-sensing neurons activate the sympathetic nervous system.
Hormones released include:
- Adrenaline
- Noradrenaline
- Cortisol
- Glucagon
The NIH explains glucose counterregulation as the body’s protective response to declining blood sugar.
Adrenaline causes trembling and rapid heartbeat. Cortisol supports longer-term glucose release.
The combination of low fuel and stress hormones makes blood sugar crash symptoms feel urgent and dramatic.
Why Blood Sugar Crash Symptoms Can Happen Without Diabetes
Many assume only people with diabetes experience crashes. In reality, healthy adults often experience reactive drops.
Triggers include:
- High-carb meals without protein
- Sugary drinks
- Long fasting gaps
- Excess caffeine
If you’re looking for alternatives to caffeine spikes, see midday energy boost without coffee.
Experiencing blood sugar crash symptoms does not automatically mean disease. It often indicates unstable meal composition.
The Link Between Blood Sugar Crashes and Mood Changes
Glucose affects neurotransmitters like serotonin and dopamine.
Low glucose availability can contribute to irritability and emotional reactivity.
If crashes consistently occur in the afternoon, consider adding structured habits from midday healthy habits to fight energy slumps.
Stabilizing blood sugar often improves mood stability.
How Exercise Influences Blood Sugar Crash Symptoms
Exercise improves insulin sensitivity and glucose uptake.

However, intense workouts without adequate fueling can provoke crashes.
Helpful strategies include:
- Pre-workout protein
- Balanced post-workout meal
- Gentle post-meal walking
- Proper hydration
Hydration plays a key role. See simple daily hydration habits for energy for support strategies.
How to Prevent Blood Sugar Crash Symptoms Naturally and Safely
Preventing blood sugar crash symptoms requires slowing glucose absorption and moderating insulin response.
5-Step Blood Sugar Stabilization Protocol
1. Pair carbohydrates with protein
Protein slows glucose absorption.
2. Increase fiber intake
Fiber reduces glycemic load.
3. Avoid liquid sugar calories
Liquid sugar spikes rapidly.
4. Maintain consistent meal timing
Avoid long fasting gaps.
5. Prioritize sleep and stress regulation
Sleep improves insulin sensitivity.

Example balanced day:
Breakfast: Eggs + whole grain toast + berries
Lunch: Lean protein + vegetables + quinoa
Snack: Apple + peanut butter
Dinner: Protein + vegetables + healthy fat
Light post-meal walking can further reduce glucose spikes.
If blood sugar crash symptoms are severe, frequent, or include confusion or fainting, seek medical evaluation.
Stable glucose supports stable energy, mood, and focus. When you stabilize blood sugar, you reduce the likelihood of repeated blood sugar crash symptoms and create a more predictable daily rhythm.
The Biological Timeline of Blood Sugar Crash Symptoms From Spike to Drop
To fully understand blood sugar crash symptoms, it helps to visualize the timeline inside your body.
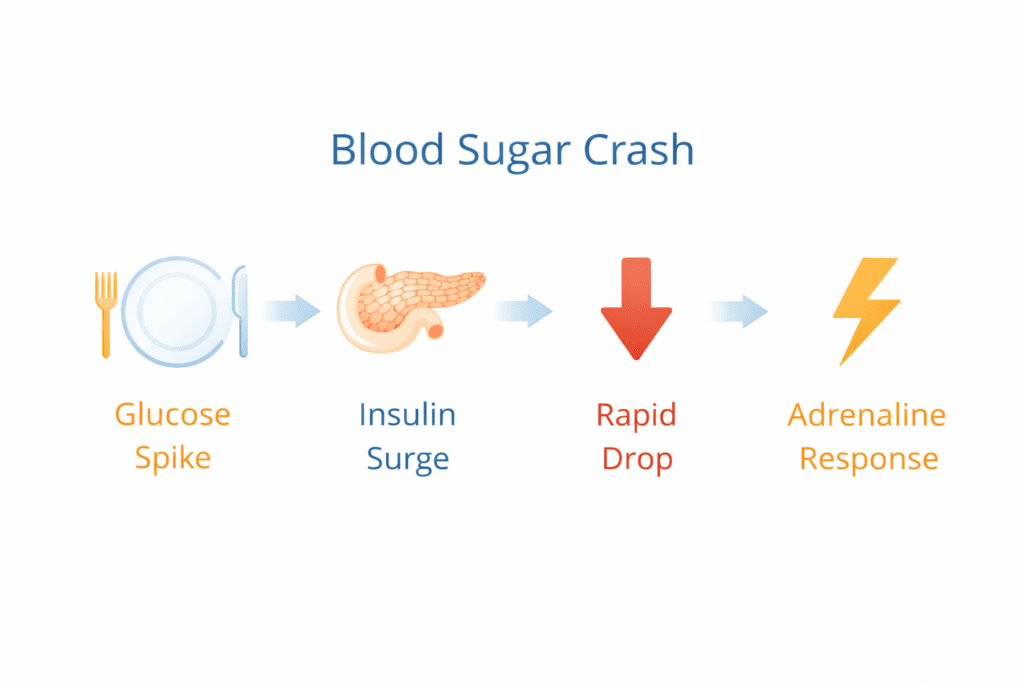
Stage 1: Rapid Glucose Spike (0–60 minutes after eating)
You consume a high-glycemic meal — white rice, sugary cereal, soda, pastries, sweetened coffee drinks. These carbohydrates digest quickly, entering the bloodstream as glucose.
Blood sugar rises sharply.
At this point, you may feel energized, alert, or even slightly wired.
Stage 2: Insulin Surge (30–90 minutes)
The pancreas releases insulin to clear glucose from the bloodstream. If the spike was steep, insulin release may also be strong.
Insulin acts efficiently — sometimes too efficiently.
Stage 3: Rapid Decline (1–3 hours later)
Glucose levels drop quickly. In some people, they fall below baseline before stabilizing.
This is when blood sugar crash symptoms begin.
You may notice:
- Sudden hunger
- Shakiness
- Irritability
- Brain fog
- Sweating
- Fatigue
If this drop happens in the afternoon, it may overlap with what feels like an afternoon energy crash, but the mechanism here is specifically glucose-driven.
Stage 4: Counterregulatory Hormone Activation
The body responds defensively. Adrenaline rises. Cortisol increases. Glucagon signals the liver to release stored glycogen.
The intensity of blood sugar crash symptoms comes from this stress-hormone activation — not just low glucose itself.
For a full breakdown of why afternoon fatigue happens, read: Why Am I So Tired in the Afternoon?
Why High-Carb Breakfasts Often Trigger Mid-Morning Crashes
Many people unknowingly create unstable glucose patterns starting with breakfast.
A common pattern:
Bagel + flavored latte
Sweetened oatmeal + juice
Granola + sweetened yogurt
These meals are carb-dominant and often low in protein and fiber.
Without protein and fat to slow absorption, glucose rises quickly. Insulin responds strongly. Blood sugar crash symptoms may appear by 10:30 or 11:00 AM.
This explains why some people feel hungry again just a couple of hours after eating.
If this sounds familiar, compare your experience to common patterns discussed in why do I feel tired after eating.
The solution isn’t eliminating carbohydrates — it’s restructuring them.
For example:
Instead of cereal alone → Eggs + whole grain toast + berries
Instead of sweetened yogurt → Greek yogurt + nuts + chia seeds
The protein and fiber reduce spike magnitude, decreasing the likelihood of blood sugar crash symptoms.
The Role of Glycemic Index and Glycemic Load in Crash Risk
Not all carbohydrates affect blood sugar equally.
The glycemic index (GI) measures how quickly a food raises blood glucose.
The glycemic load (GL) considers both the GI and the amount of carbohydrate consumed.
High GI + high portion size = greater spike potential.
According to Harvard Health’s explanation of glycemic index and glycemic load, foods with a high glycemic index tend to raise blood sugar more quickly and more dramatically than low‑glycemic foods, and foods with a high glycemic load produce faster and larger glucose rises after eating.
Examples of higher spike foods:
- White bread
- Sugary drinks
- Candy
- White rice
- Refined cereals
Lower glycemic impact foods:
- Lentils
- Beans
- Vegetables
- Whole intact grains
- Nuts
Choosing lower glycemic combinations reduces the steep rise that precedes blood sugar crash symptoms.

How Caffeine Can Mask and Then Amplify Blood Sugar Crash Symptoms
Caffeine stimulates adrenaline.
If consumed on an empty stomach, caffeine may temporarily mask fatigue by increasing alertness. But it does not stabilize glucose.
In fact, caffeine can:
- Increase cortisol
- Slightly raise blood glucose
- Increase insulin demand
When the caffeine effect fades, you may experience:
- Increased fatigue
- Shakiness
- Irritability
This can feel like blood sugar crash symptoms — or worsen an existing glucose drop.
If you rely on multiple coffees daily to counter fatigue, review strategies in midday energy boost without coffee.
Why Long Gaps Between Meals Increase Crash Severity
Skipping meals or delaying eating for long periods can destabilize glucose regulation.
When you go many hours without food:
- Liver glycogen stores decline
- Cortisol rises
- The body becomes more sensitive to the next glucose spike
If the next meal is carb-heavy, insulin response may be exaggerated.
This increases the likelihood of blood sugar crash symptoms.
Some people report feeling extremely shaky after finally eating following a long fasting window. This reflects a dramatic swing rather than stable regulation.
Consistency often matters more than strict restriction when trying to prevent crashes.
Blood Sugar Crash Symptoms and Sleep Disruption
Unstable glucose can affect nighttime stability.
If blood sugar drops during sleep, adrenaline may rise. You may wake:
- Around 2–3 AM
- With a racing heart
- Feeling anxious
- Unable to fall back asleep

This pattern overlaps with experiences described in wired but tired at night.
Stabilizing dinner composition — ensuring adequate protein and fiber — can reduce nocturnal variability.
Sleep and glucose regulation are bidirectional:
Poor sleep worsens insulin sensitivity.
Unstable glucose disrupts sleep.
Improving one supports the other.
The Connection Between Stress Hormones and Glucose Instability
Chronic stress elevates cortisol.
Cortisol increases glucose availability by stimulating liver glucose production. While this is adaptive short term, chronic elevation can create irregular glucose patterns.
High stress may:
- Increase cravings
- Disrupt appetite signals
- Increase insulin resistance
- Amplify blood sugar crash symptoms
This explains why crashes may feel worse during high-pressure periods at work.
Incorporating stress-reducing strategies such as those outlined in daily rituals to reduce stress and improve mood and energy can indirectly improve glucose stability.
Why Some People Experience Shakiness Without Severe Hypoglycemia
Many individuals experiencing blood sugar crash symptoms do not meet the medical threshold for hypoglycemia.
Clinical hypoglycemia is generally defined as blood glucose below 70 mg/dL.
However, rapid drops — even within normal range — can trigger symptoms.
The speed of decline matters.
A fall from 160 mg/dL to 85 mg/dL in a short period may trigger:
- Trembling
- Anxiety
- Weakness
even though 85 mg/dL is technically normal.
This is called relative hypoglycemia.
The nervous system responds to rate of change, not just absolute number.
How Muscle Mass Improves Glucose Buffering
Muscle tissue acts as a storage reservoir for glucose.
More muscle mass improves glucose uptake efficiency.

Strength training increases:
- GLUT4 transporter activity
- Insulin sensitivity
- Glycogen storage capacity
This reduces spike amplitude and lowers risk of blood sugar crash symptoms.
Even simple strength routines such as those in 10-minute no-equipment leg workouts can contribute to improved metabolic stability over time.
Muscle is metabolically protective.
Real-Life Scenario: The Office Worker Crash Pattern
Consider this common pattern:
8:00 AM – Sweet coffee + pastry
12:30 PM – White rice bowl + soda
3:00 PM – Severe fatigue and shakiness
4:00 PM – Candy bar
8:00 PM – Heavy dinner
This creates repeated glucose swings throughout the day.
By 3 PM, what feels like random exhaustion may actually be blood sugar crash symptoms layered onto natural circadian dip.
This pattern overlaps with the experience described in exhausted at 3PM even after 8 hours sleep, but here the dominant mechanism is glucose variability.
Replacing pastry with protein breakfast and adding balanced afternoon snack dramatically reduces instability.
Long-Term Metabolic Consequences of Repeated Spikes and Crashes
Frequent glucose spikes followed by crashes can:
- Increase insulin demand
- Promote fat storage
- Increase appetite signaling
- Reduce metabolic flexibility
Over time, this may contribute to insulin resistance.
Stable glucose curves protect long-term metabolic health.
Blood sugar crash symptoms are short-term discomfort signals — but the underlying instability may have long-term implications if ignored.
Advanced Stabilization Strategy: Building a “Low-Variability Plate”
To reduce blood sugar crash symptoms consistently, use a simple structural model:
½ plate non-starchy vegetables
¼ plate protein
¼ plate complex carbohydrate
Add healthy fat
This combination slows glucose absorption and moderates insulin response.
Example:
Grilled chicken
Roasted vegetables
Quinoa
Olive oil
This structure flattens the glucose curve.
Add 10-minute post-meal walk for additional stability.
When to Seek Medical Evaluation for Blood Sugar Crash Symptoms
Occasional moderate crashes are common.
However, medical evaluation is important if symptoms include:
- Confusion
- Fainting
- Blurred vision
- Seizures
- Frequent severe episodes
The Mayo Clinic advises evaluation for recurrent hypoglycemia symptoms.
If episodes are severe or frequent, testing may be needed.
Final Integration: Why Stable Glucose Means Stable Energy
Blood sugar crash symptoms are not random. They are physiological signals that glucose regulation is unstable.
When you stabilize:
- Meal composition
- Fiber intake
- Protein intake
- Sleep
- Stress
- Physical activity
you reduce variability.

Reduced variability means:
- Fewer cravings
- More predictable mood
- Clearer thinking
- Steadier energy
Stable glucose supports stable daily rhythm.
Blood sugar crash symptoms improve when glucose curves flatten.
Energy becomes consistent instead of reactive.
Ready to Stop Blood Sugar Crashes for Good?
Start stabilizing your energy with simple, science-backed habits. Get personalized strategies for keeping your blood sugar in balance throughout the day.
- Afternoon Energy Crash Prevention: The Simple Habits You Need
- Boost Your Midday Energy Without Coffee
- 7 High-Protein Snacks Under 200 Calories to Prevent Crashes
Want a step-by-step plan to avoid the afternoon slump? Follow our Midday Energy Reset Plan to keep your blood sugar levels stable and feel energized all day.
Get the Midday Energy Reset ChecklistFrequently Asked Questions
What are blood sugar crash symptoms?
Blood sugar crash symptoms include shakiness, sudden fatigue, brain fog, sweating, irritability, rapid heartbeat, and intense hunger. These symptoms occur when glucose levels drop quickly after a spike, triggering stress hormones like adrenaline and cortisol.
What causes blood sugar crash symptoms?
Blood sugar crash symptoms are usually caused by a rapid rise in glucose followed by an exaggerated insulin response. High-glycemic meals, sugary drinks, low-protein meals, long gaps between eating, poor sleep, and stress can all contribute to unstable glucose levels.
What does a blood sugar crash feel like?
A blood sugar crash often feels like sudden weakness, trembling, anxiety, difficulty concentrating, and urgent hunger. Many people describe it as feeling shaky and exhausted at the same time due to low glucose combined with adrenaline release.
How long do blood sugar crash symptoms last?
Mild blood sugar crashes typically last 20–60 minutes and improve after eating a balanced meal or snack. More severe crashes may last longer, especially if not addressed with proper nutrition that includes protein and fiber.
Can you have blood sugar crash symptoms without diabetes?
Yes. Blood sugar crash symptoms can occur in people without diabetes. Reactive hypoglycemia, which happens a few hours after eating, may develop in healthy adults after consuming high-carbohydrate meals without enough protein or fiber.
Why do I feel shaky a few hours after eating?
Feeling shaky a few hours after eating is often caused by a rapid insulin response that lowers blood sugar too quickly. This triggers adrenaline release, which causes trembling, sweating, and sudden fatigue.
Is a blood sugar crash the same as hypoglycemia?
Not always. A blood sugar crash may involve a rapid drop in glucose without reaching clinical hypoglycemia levels. True hypoglycemia usually refers to blood sugar below 70 mg/dL, while relative drops can still cause noticeable symptoms.
Why do blood sugar crash symptoms feel like anxiety?
Blood sugar crashes activate the sympathetic nervous system, releasing adrenaline. This stress hormone causes symptoms such as racing heart, sweating, shakiness, and nervousness, which closely resemble anxiety or panic attacks.
Can poor sleep cause blood sugar crash symptoms?
Yes. Sleep deprivation reduces insulin sensitivity and disrupts glucose regulation. Poor sleep can increase blood sugar variability during the day, making crashes more likely after meals.
How can I prevent blood sugar crash symptoms naturally?
You can prevent blood sugar crash symptoms by pairing carbohydrates with protein, increasing fiber intake, avoiding sugary drinks, maintaining consistent meal timing, managing stress, and prioritizing quality sleep. Light post-meal walking also helps stabilize glucose levels.
What foods help prevent blood sugar crashes?
Foods that help prevent crashes include lean protein, vegetables, legumes, whole grains, nuts, seeds, and healthy fats. Balanced meals slow glucose absorption and reduce insulin spikes.
Are blood sugar crashes dangerous?
Occasional moderate crashes are usually not dangerous in healthy adults. However, severe symptoms such as confusion, fainting, blurred vision, or frequent episodes require medical evaluation.
About This Content
This article integrates evidence-based physiology of glucose metabolism, insulin regulation, and counterregulatory hormone response as described by institutions such as the NIH, Mayo Clinic, Harvard Health, and Cleveland Clinic. It focuses on educational explanation, not medical diagnosis, and is designed to support informed lifestyle adjustments for stable daily energy.
